Crossmodal Illusions in neurorehabilitation – other perspectives –

Authors: Livia Popa, Victor Dabala, Oana Vanta
Keywords: crossmodal illusions, sensory signals, neurorehabilitation, rubber hand illusion, mirror box illusion
- What are crossmodal illusions in neurorehabilitation?
- Mirror Box Illusion & Neurorehabilitation
- Mirror Box Illusion and phantom limb pain (PLP)
- Mirror Box Illusion and chronic pain of central origin
- Mirror Box Illusion and complex regional pain syndrome
- Mirror Box Illusion and motor cortex trasncranial direct current stimulation (tDCS)
- Mirror Box Illusion and rehabilitation of hemiparesis in stroke patients
- Rubber Hand Illusion
- Conclusions
- References
What are crossmodal illusions in neurorehabilitation?
As human beings, we are surrounded every minute by a multitude of external and internal stimuli; thus, our brain is permanently stimulated. Those specific stimuli converge into discrete brain areas, and the brain ultimately synthesizes unified percepts. Even though vision seems to be the dominant sense, the brain can differentiate and process simultaneously different sensory signals. In this way, perceptual and cognitive functions and the underlying brain activity are shaped by interactions between senses without any conscious effort. The brain’s specialized neural and cortical mechanisms synthesize the sensory information from the different senses into coherent, unitary representations that guarantee adaptive behavioral responses [1].
The sensorial systems are specifically designed to recognize different stimuli at every moment of our life, and capable of perceiving more than a single signal at a specific time. These signals are further integrated at upper levels without involving consciousness, causing an interrelation that models certain aspects of the brain functions. A significant advantage of a multimodal synthesis is the augmentation of the responsiveness to the stimuli received, causing the facilitation of the effector response like:
- fastening spatial orienting;
- improving memory and language comprehension;
- optimizing sensorimotor control [1].
When the structures responsible for analyzing the stimuli come across incoherent information, the information itself tends to get organized in a manner that causes crossmodal illusions. Crossmodal illusions (CMI) can be defined as the impact produced in one modality caused by the perception of a different modality. Therefore, this mechanism is responsible for resolving uprising conflicts generated by inter-sensory processes [1, 2].
Two proposed processes explain the influence of multimodality on perception, as described in Figure 1 below [1, 2]:

Crossmodal illusions have been successfully applied in certain domains of neurology, like neuropsychology, observing a possible impaired mechanism for integrating multiple stimuli in patients with acquired focal brain lesions. The beneficial effects of CMI are more prevalent in patients with brain diseases, a category that is more susceptible to multimodal illusions -hence their sensory or motor impairment [1, 2].
The review conducted by Bolognini et al. [3] considered the fascinating field of research concerned with the possibility of using crossmodal illusions as tools for rehabilitation. The authors focused on the Mirror Box and the Rubber Hand illusions, the two most renowned and common crossmodal illusions used in clinical practice to treat pain (especially phantom limb syndrome), post-stroke impairments, and in neuroprosthetics [3].
The efficacy of crossmodal illusions has been established in several clinical aspects mentioned in Figure 2 below [3]:

Mirror Box Illusion & Neurorehabilitation
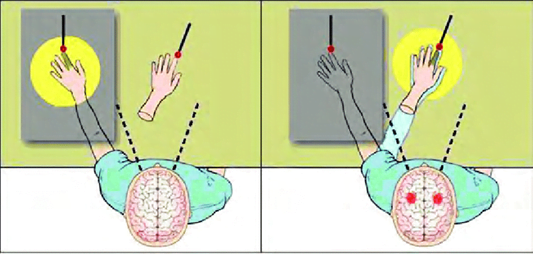
The Mirror Box Illusion (MBI), one of the most famous CMI, has a visual-motor conflict at its root. While one hand is maintained behind the mirror, concealed from view, participants move the other hand in front of a parasagittal mirror. On the hidden limb, they may perceive symmetrical bimanual movements and other deceptive kinaesthetic and motor effects (see Figure 3). Thus, observing one’s own actions in the mirror enhances excitability in the motor cortex ipsilateral to the moving hand.

The mismatch between the movement individuals do and the movement they perceive increases neuronal activity in brain areas involving self-awareness and spatial attention, more specifically:
- the precuneus,
- posterior cingulate gyrus,
- posterior parietal cortices [1].
Clinical applications of MBI (as seen in Figure 4 below) are mainly related to pain management [3].

Mirror Box Illusion and phantom limb pain (PLP)
The MBI was first used in clinical trials to treat Phantom limb pain (PLP) following amputation.
Melzack (1992) was the first to argue that the so-called “neuromatrix” plays a crucial role in the development of the body image and the creation of pain [5].
Patients report feeling able to move and relax the cramped phantom limb and experiencing pain alleviation when the intact arm overlays the phantom limb through a mirror reflection.
In this theory, relief from PLP results from the visual input of movements of the missing limbs correcting the incongruence between motor output (intention) and sensory (proprioceptive) feedback. As a result, the missing limb’s “latent” cerebral map may be reactivated [3, 6].
Mirror Box Illusion and chronic pain of central origin
Furthermore, the MBI’s sensory-motor conflict can affect motor cortical excitability, which is changed in many individuals with chronic pain of central origin.
However, moving the phantom limb does not always reduce PLP; phantom movement increases PLP (cramping sensations) in some amputees [6]. Consequently, an alternative version of the MBI has been devised, in which patients look at the mirror reflection of touches administered to the intact hand while receiving touches on the stump behind the mirror [7].
Mirror Box Illusion and complex regional pain syndrome
MBI has been used successfully in patients with complex regional pain syndrome and even in sensory re-education of acute hyperesthesia following hand injuries [8].
Chronic pain is linked to maladaptive neuroplastic changes in the brain. Impaired or altered multisensory processing can be modulated by the MBI’s sensory-motor conflict [3].
Mirror Box Illusion and motor cortex trasncranial direct current stimulation (tDCS)
One recent advancement in MBI for pain treatment is its usage in conjunction with motor cortex transcranial direct current stimulation (tDCS). Different physiological processes, which share some similarities with those of the MBI, mediate the analgesic action of motor cortex stimulation by tDCS, including regulation of motor cortex excitability and alterations in perceptual and emotional processing of the pain experience [9].
Using tDCS as a supplement to MBI could enhance its analgesic effects. tDCS over the motor cortex was provided during a modified version of the MBI, which consisted of a virtual reality method to produce the visual illusion of walking in patients with neuropathic pain following spinal cord injury. Combining tDCS and MBI reduced overall pain severity and improved different subtypes of neuropathic pain- continuous and paroxysmal pain, mechanical allodynia, and dysesthesia, with stronger and longer-lasting effects than either intervention alone (tDCS or MBI) [10].
Mirror Box Illusion and rehabilitation of hemiparesis in stroke patients
The MBI’s rehabilitation of hemiparesis in stroke patients is another well-known use.
Monitoring self-induced motions in the left side of space may help with leftward visuospatial orienting, which is hindered due to left spatial neglect. Evidence of the MBI’s favorable effects on unilateral visuospatial neglect further supports this idea [11].
In recent years, the Mirror Box Illusion has been applied for a specific condition called the alien hand syndrome (AHS). The movement process in AHS is described as involuntary, with a certain degree of deliberate initiative. Several etiologies are considered, like brain infarction (especially following the occlusion of the Anterior Cerebral Artery, midline tumors, or neurodegenerative diseases. The main benefit of the MBI appliance in AHS was reestablishing the connection between the initiation of the motor action and the visual response with the improvement of the voluntary fine motor control of the alien hand [12].
Rubber Hand Illusion
Another crossmodal method highlighted in the review of Bolognini et al. [3], which is still in the early stages when referring to neurorehabilitation, Rubber Hand Illusion (RHI), consists of brushing one of the subject’s hands (not visible to the observer) while the examiner brushes a specific rubber-based hand simultaneously. Therefore, a sense of ownership is generated for the patient [3].
Principles behind RHI:
- elevation of the patient’s proprioceptive function;
- changes in reaching movements performed with the stimulated hand;
- the connection between body representation and the multimodal integration of touch, proprioception, and visual stimuli (Figure 5).
The clinical applications of Rubber Hand Illusion :
-Somatoparaphrenia
-Visuospatial neglect
– Complex Regional Pain Syndrome
-Cervical Spinal Cord Injury
– Neuroprosthetics
The primary appliance for RHI is considered somatoparaphrenia – a bodily illusion in which the patient feels disownership of the contralesional body, frequently caused by right-hemispheric damage, and appears to be closely associated with unilateral spatial neglect.
An alternative version of the RHI, in which both hands, with the right hand, are concealed and the left one considered disowned by the patients suffering from somatoparaphrenia. The second variant allows the subject to readjust their sense of ownership over the unrecognizable hand, restoring the multisensory integration and projection of the body [3].
RHI is also associated with several other disorders, like Complex Regional Pain Syndrome and Cervical Spinal Cord Injury.
The mechanisms of action of RHI for those two pathologies rely on the improvement in the fields of tactile awareness and processing, the reactivation of tactile memories, restoration of a coherent bodily self-representation, and also relief of chronic pain linked with these conditions [3].
RHI can also be a solution for patients suffering from visuospatial neglect with benefits like strengthening spatial and body awareness, the recovery of spatial attention deficits, and modifying the brain’s visuomotor mapping [2].
RHI is considered a milestone in the field of neuroprosthetics, causing an illusion of touch by stroking both the stump and the fingers at the same moment. The actions performed lead to activating both the premotor cortex and certain parietal regions, generating a sense of ownership over the phantom limb. The main result of the RHI appliance in neuroprosthetics can be considered the improvement of cortical plasticity [7].
The are other crossmodal illusions used in clinical settings, but not yet in rehabilitation, like :
- The Ventriloquism illusion – Hemianopia and neglect;
- The Aristotle’s illusion – Focal hand dystonia;
- The Sound-induced flash illusion – Migraine [3].
Conclusions
Bolognini et al. [3] concluded in the short review that by integrating CMI and inter-sensory conflicts in the current rehabilitation practice, several significant advantages could be obtained like the improvement in multisensorial capabilities, restoration of body awareness, regaining body ownership, increased movement capacity, retrain sensibility and attention focus and decrease the intensity of neuropathic/chronic pain [3].
Cross-modal illusions have been described as beneficial for augmentation of the multisensorial aspects following a debilitating condition (e.g. ischemic stroke). The assimilation of different stimuli simultaneously is conserved concerning the appliance of illusions, opening an unconventional pathway in the vast domain of neurorehabilitation. While the current body of literature cannot be considered abundant, the modulation of multisensorial inputs in the impaired brain should be further investigated about the positive results observed after the appliance of cross-modal illusions.
References
- Driver J, and Noesselt T. Multisensory interplay reveals crossmodal influences on ‘sensory-specific’brain regions, neural responses and judgments. Neuron 2008; 57, 11–23. DOI: 10.1016/j.neuron.2007.12.013
- Bolognini N, Convento S, Rossetti A, Merabet LB. (2013a). Multisensory processing after a brain damage: clues on post-injury crossmodal plasticity from neuropsychology. Neurosci. Biobehav. 2013a; Rev. 37, 269–278. https://doi.org/10.1016/j.neubiorev.2012.12.006
- Bolognini N, Russo C and Vallar G. Crossmodal illusions in neurorehabilitation. Front Behav Neurosci 2015; 9:212. https://doi.org/10.3389/fnbeh.2015.00212
- Ghoseiri K, Allami M, Soroush MR, and Rasthadiv MY. Assistive technologies for pain management in people with amputation: a literature review. Military Med Res 2018; 5, 1. https://doi.org/10.1186/s40779-018-0151-z
- Melzack R. Phantom limbs. Sci. Am 1992;. 266, 120–125. DOI: 10.1038/scientificamerican0492-120
- Ramachandran, VS, Rogers-Ramachandran D, and Cobb S. (1995). Touching the phantom limb. Nature 1995; 377, 489–490. DOI: 10.1038/377489a0
- Schmalzl L, Ragnö C, and Ehrsson HH. An alternative to traditional mirror therapy: illusory touch can reduce phantom pain when illusory movement does not 2013. Clin. J. Pain 29, e10–e18. DOI: 10.1097/AJP.0b013e3182850573
- Moseley GL, Gallace A, and Spence C. Is mirror therapy all it is cracked up to be? Current evidence and future directions. Pain 2008; 138, 7–10. DOI: 10.1016/j.pain.2008.06.026
- Brunoni AR, Nitsche MA, Bolognini N, Bikson M et al. Clinical research with transcranial direct current stimulation (tDCS): challenges and future directions. Brain Stimul. 2012; 5, 175–195. DOI: 10.1016/j.brs.2011.03.002
- Soler MD, Kumru H, Pelayo R, Vidal J et al. Effectiveness of transcranial direct current stimulation and visual illusion on neuropathic pain in spinal cord injury. Brain 2010; 133, 2565–2677. https://doi.org/10.1093/brain/awq184
- Dohle C, Püllen J, Nakaten A, Küst J, Rietz C, and Karbe H. Mirror therapy promotes recovery from severe hemiparesis: a randomized controlled trial. Neurorehabil. Neural Repair 2009; 23, 209–217. DOI: 10.1177/1545968308324786
- Romano D, Sedda A, Dell’Aquila R, Dalla Costa D et al. Controlling the alien hand through the mirror box. A single case study of alien hand syndrome. Neurocase 2014; 20, 307–316. https://doi.org/10.1080/13554794.2013.770882
- Metzinger T. Empirical perspectives from the self-model theory of subjectivity: a brief summary with examples. Prog Brain Res 2008; 168:215-45. DOI: 10.1016/S0079-6123(07)68018-2










thanks for info.