Neurorehabilitation in dystonia – a holistic approach

Authors: Irina Benedek, Livia Popa, Oana Vanta
Keywords: dystonia, cervical dystonia, rehabilitation, motor symptoms, non-motor symptoms
Neurorehabilitation in dystonia
First of all we should define dystonia. So, what is actually dystonia? Dystonia is an uncontrollable, persistent, or intermittent muscular contraction that affects one or more body parts and results in aberrant postures, repetitive motions, tics, or tremors [1]. The most prevalent idiopathic isolated cervical dystonia (CD) affects the head and neck, where motor dysfunction and discomfort result in considerable suffering and impairment [2].
Despite patients’ low satisfaction, regular botulinum toxin injections (BoNT) remain the most often prescribed medical therapy for CD. With varying degrees of effectiveness, rehabilitation by allied health practitioners often entails neck exercises to strengthen antagonist muscles and diminish pathological activity in constricted muscles [3].
Different rehabilitation strategies have been used for dystonia:
- botulinum toxin injections
- anticholinergic drugs
- deep brain stimulation.
While there is growing evidence of non-motor symptoms like pain, fatigue, sleep, and mood disorders that further restrict daily life functions and have a negative impact on quality of life, motor symptoms like head tremors, abnormal posture, and jerks are considered to be the most troublesome (Figure 1) [3]. Recent research demonstrating functional, gait, and balance impairments suggests the need for a more comprehensive rehabilitation strategy [4]. The significant dysfunctions besides the dystonic body parts and their significance for comprehensive therapy are outlined in the study by Bradnam et al. [3].
Physical function, gait, and balance disorders in patients suffering from dystonia
Physical function is impaired in CD patients, which is not surprising given the critical role that proprioception, visual, and vestibular functions play in sustaining upright posture and balance. The head-turn posture affects how the central nervous system (CNS) processes sensory information from all three systems. Therefore, physical evaluations of individuals with dystonia should include the following:
- postural control evaluation
- gait function evaluation [3].
When spatiotemporal parameters are assessed in a laboratory setting, emerging data show that persons with CD have gait impairment and walk more slowly [5].
Ten CD patients and ten normal individuals were compared regarding various gait kinematic measurements utilizing an instrumented walkway. Average step length and step duration were lowered and increased, respectively, in the dystonia group. Patients also spent more time in double support (both feet on the ground), which is an effect of poor balance control. To support this, CD doubled the time required to complete the timed-up-and-go (TUG) test, a standard physical function assessment tool involving gait speed, turning, and balancing [5].
Reduced cervical range of motion (neck flexion) was significantly correlated with delayed simple and choice reaction times and increased postural sway. In contrast, limited cervical rotation was connected to a slower TUG completion time, suggesting that the functional deficits may be caused by abnormal head posture. The correlations between the cervical range of motion and functional measures are illustrated in Figure 1 [5].
Currently, the treatment of cervical dystonia focuses mainly on the affected cervical area. However, the data summarised showed the usefulness of including:
- physical function tests
- postural control
- and/or stepping reaction exercises, together with gait rehabilitation, in the therapeutic care of dystonia [3].
Falling and fear of falling – concepts and management
People with dystonia may be affected in ways that might lead to falls due to problems of gait, balance, and vision. To learn more about the experience of falling for this category of patients, the authors carried out an international survey of a diverse dystonic population. Of the 122 respondents, 39% reported falling over in the preceding six months. In contrast to dystonia which directly affected the trunk and/or lower limbs, several fallers suffered from isolated types of dystonia such as:
- Cervical Dystonia
- Blepharospasm
- Focal hand dystonia [6].
This demonstrated that dystonia’s effects on physical function, like decreased sensorimotor control, balance, and gait, are factors that may lead to falling [6].
Previous research results showcase that fallers exhibited a noticeably higher fear of falling and worse balance confidence than those who did not fall [6]. The authors implemented the Activities-Specific Balance Confidence Scale (ABC) and the Falls Self-Efficacy Scale-International (FES-I) for the assessment of the study population and determined cut-off points for the risk of falls.
The patients who responded to the survey listed various causes for falling. Losing balance when walking, turning, reaching, or using stairs was the most frequent cause. It was also common to fall after tripping, which was frequently associated with CD or blepharospasm-induced impaired vision (BLP) [6].
In a recent prospective research, Boyce and colleagues looked at functional balance and walking tests in CD adults using scales verified in other neurological groups or in older, healthy individuals. According to early research, CD patients generally performed well on the physical functional scores, revealing that balance and movement may not be as compromised as previously suggested. As a result, it is probable that psychological issues (anxiety, depression, stigma, fear of movement, etc.) rather than physical limits are to blame for the previously observed fear of falling [7].
Although this theory is hypothetical and needs further research, it significantly influences how dystonia patients are treated during post-fall rehabilitation. In these situations, boosting balance confidence from a psychological perspective may have a greater impact than physical or exercise-based rehabilitation. Regardless, falls-related anxiety should be handled from a multidisciplinary point of view, and rehabilitation programs should incorporate fall prevention most suitably based on thorough physical and psychological assessments [3].
Visual impairment in dystonic patients
People with CD have more postural sway while their eyes are open compared to control adults; this suggests that vision is not employed as much as it should be to keep the center of gravity within the base of support. Undoubtedly, eye impairment brought on by dystonic postures is a significant problem for many CD patients [3].
Reduced vision-related quality of life was demonstrated in a study of 42 patients conducted by Bradnam and colleagues, which compared mixed dystonia to normative data. Ocular symptoms and role performance, two areas of a questionnaire measuring the vision-related quality of life, were substantially different among people with dystonia. They discovered that one young female participant (out of ten) had significant visuospatial neglect utilizing a battery of computer-based and manual spatial neglect tests, indicating that neurological vision abnormalities should also be taken into account in CD. Clinicians should be aware that their CD patients may suffer neglect, and a thorough examination of dystonia should include testing for this matter [8].
The comprehensive treatment of dystonia should take into account visual impairment brought on by dystonic postures and its effects on:
- physical function;
- visual compensation;
- oculomotor fatigue;
- spatial neglect [3].
When experiencing life contexts that require visual compensation for a rotated neck, such as crossing a busy road, persons with CD may experience oculomotor fatigue that might have an impact on their safety. In order to make the required adjustments, clinicians and patients should both be aware of the possibility of oculomotor fatigue related to recurrent eye movements in the opposite direction to head motion [3].
Non-motor symptoms associated with dystonia
When approaching the comprehensive rehabilitation of dystonia, it is crucial to consider non-motor symptoms since they significantly impact the quality of life. Non-motor symptoms that cause impairment and limit everyday activities are common in this category of patients [3].
Figure 2 shows the motor and non-motor symptoms of dystonia. While motor symptoms are frequently thought of as the primary issue that needs to be resolved, there are a great number of additional, less obvious symptoms that significantly impact a person’s level of disability and quality of life [3].
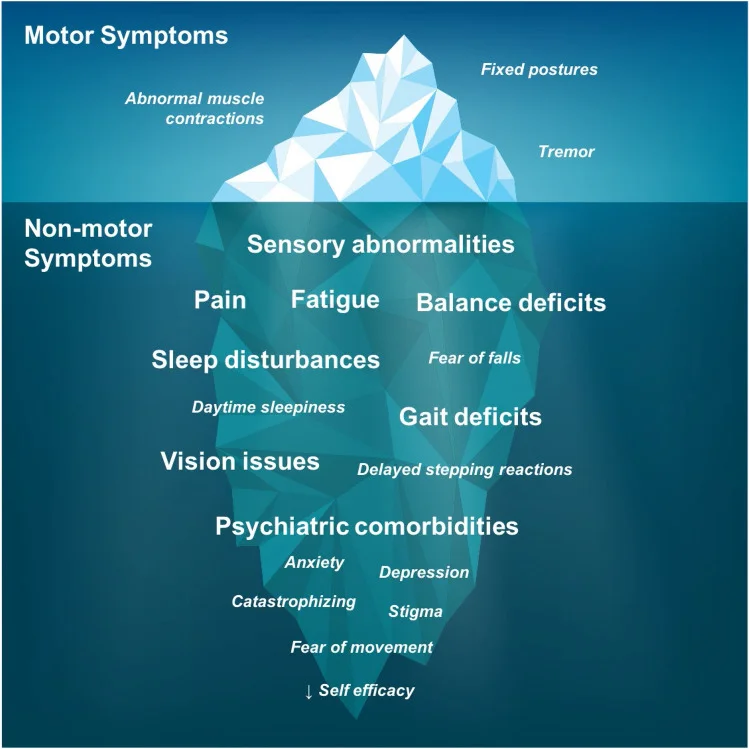
- Dystonia is characterized by a common and crippling non-motor symptom of pain.
Pain is experienced by 55-89% of patients with CD. Despite being a frequent co-occurring symptom of dystonia, the mechanism underlying this discomfort is not well understood, and there are few reliable therapeutic techniques [3]. Dystonia-induced persistent muscular contractions are likely not the primary source of pain; aberrant brain processing may also be the primary culprit. The current study focused on better understanding how patients with dystonia characterize the discomfort they experience, which will be used to guide suitable therapy approaches [3]. Furthermore, BoNT and medication are the most often used treatment options for managing pain. CD pain reduction also appears promising when paired with novel cerebellar neuromodulation approaches [3].
- Whether the dystonia is focal, segmental, widespread, idiopathic, or heredodegenerative, neuropsychiatric symptoms frequently accompany it.
All types of idiopathic dystonia, including CD (up to 90% prevalence), include neuropsychiatric comorbidities that have been reported to be considerably greater than controls [3]. For many patients, psychological symptoms like anxiety and depression appear before motor symptoms, indicating they could be a basic aspect of dystonia. A proportion of individuals are likely to develop depression as a side effect of dealing with their dystonic symptoms, given the crippling sense of pain and the numerous additional symptoms that co-occur with this pathology. Studies on CD or segmental and generalized dystonia patients demonstrate that mood improves with beneficial treatment outcomes, despite the association between the severity of dystonia and the degree of depression is not evident [3].
- Fatigue is a significant problem that develops irrespective of psychological causes and sleep quality.
Exercise and physical activity engagement were shown to be significantly impaired by fatigue [3]. Research on fatigue in dystonia is essential, and fatigue management should be a part of comprehensive rehabilitation plans [3]. Moreover, sleep problems and fatigue are frequently linked; disturbed sleep is a non-motor symptom of dystonia that affects between 44 and 70% of CD and BLP patients, with research on sleep in dystonia showcasing decreased sleep efficiency and quality, reduced time spent in REM sleep, and more awakenings. Depression and anxiety are linked to poor sleep quality or excessive daytime drowsiness in dystonia [3].
Discussion and conclusion
According to the research conducted by Bradnam et al., limited efficacy and patient satisfaction are provided by current dystonia treatments. This may be because existing treatments are ineffective as they are too narrowly focused and do not account for the broader effects of dystonia on both motor performance and non-motor symptoms. Significant handicaps, detrimental effects on everyday living, and decreased quality of life are brought on by tremors and jerks, pain and exhaustion, balance and gait issues, fear of falling, visual problems, poor sleep, anxiety, and depression [3].
All of these factors should be taken into account by therapists when they start to plan a patient’s rehabilitation. The larger spectrum of dystonic signs and symptoms should be recognized and treated to improve treatment results and overall quality of life for persons with dystonia [3].
Since there is no cure for dystonia, therapists should concentrate on treating the symptoms beyond the dystonic muscular contraction. Additionally, therapists need to assess these problems before they can start offering comprehensive therapy. When evaluating a patient, physical therapists should consider testing the patient’s gait, physical function, and balance, as well as performing a clinical assessment of gait [3].
While neurorehabilitation has a place in the treatment of dystonia, a holistic rehabilitation strategy is required for addressing the wide range of motor and non-motor symptoms. The primary focus of treatment refers to the motor symptoms, such as prolonged muscular contractions, aberrant postures, tremors, and muscle jerks. However, just a small number of the crippling non-motor symptoms contribute to the lived experience of dystonia, namely pain, anxiety, stigma, disturbed sleep, and exhaustion [3].
Since non-motor symptoms have been shown to reduce health-related quality of life more than motor symptoms, rehabilitation must use a multidisciplinary approach. Future research should continue to examine the broader deficits connected to dystonia and the effects of a comprehensive rehabilitation strategy employing well-crafted multidisciplinary clinical trials [3]. Moreover, self-efficacy and self-management approaches, along with maintaining a healthy lifestyle are vital needs for ensuring long-term outcomes. Due to these reasons, self-management interventions are one important avenue to be further developed.
For more information about neurorehabilitation and stroke, visit:
- Efficacy of placebo in managing pain for neurological disorders
- Pregnancy and stroke: What are the risks and implications?
- How does gender influence stroke and neurorehabilitation?
We kindly invite you to browse our Interview category: https://efnr.org/category/interviews/. You will find informative discussions with renowned specialists in the field of neurorehabilitation.
References
- Albanese A, Bhatia K, Bressman SB, Delong MR, et al. Phenomenology and classification of dystonia: a consensus update. Mov Disord. 2013; 28(7):863-73. doi: 10.1002/mds.25475.
- Dauer WT, Burke RE, Greene P, Fahn S. Current concepts on the clinical features, aetiology and management of idiopathic cervical dystonia. Brain. 1998;121 ( Pt 4):547-60. doi: 10.1093/brain/121.4.547.
- Bradnam LV, Meiring RM, Boyce M, McCambridge A. Neurorehabilitation in dystonia: a holistic perspective. J Neural Transm (Vienna). 2021 Apr;128(4):549-558. doi: 10.1007/s00702-020-02265-0.
- Batla A, Bradnam L, Kimberley TJ (2019) Rehabilitation as a therapeutic approach for dystonia. In: Papa S (ed) MDS Scientific Issues Committee Blog. Movement Disorders Society, Milwaukee. Available from: https://www.movementdisorders.org/MDS/Scientific-Issues-Committee-Blog/Rehabilitation-as-a-Therapeutic-Approach-for-Dystonia.htm
- Barr C, Barnard R, Edwards L, Lennon S, Bradnam L. Impairments of balance, stepping reactions and gait in people with cervical dystonia. Gait Posture. 2017 Jun;55:55-61. doi: 10.1016/j.gaitpost.2017.04.004.
- Boyce MJ, Lam L, Chang F, Mahant N, et al. Validation of Fear of Falling and Balance Confidence Assessment Scales in Persons With Dystonia. J Neurol Phys Ther. 2017;41(4):239-244. doi: 10.1097/NPT.0000000000000198.
- Boyce MJ, Chang FCF, Mahant N, Fung VSC, Bradnam L. A survey of falls in people with dystonia. Physiother Res Int. 2020;25(3):e1840. doi: 10.1002/pri.1840.
- Bradnam L, Chen C, Graetz L, Loetscher T. Reduced vision-related quality of life in people living with dystonia. Disabil Rehabil. 2020 Jun;42(11):1556-1560. doi: 10.1080/09638288.2018.1528636.









