Shedding light on Speech-Language Therapy: How stroke survivors can benefit from intensive rehabilitation training for chronic aphasia

Authors: Victor Dabala, Oana Vanta
Keywords: chronic aphasia, intensive training, randomized controlled trial, Intensive Language Action Therapy, Speech-Language Therapy
Speech-Language Therapy – A constant source of debate
While Speech-Language Therapy (SLT) is considered a vital rehabilitation method in treating post-stroke aphasia, question marks regarding the necessary time and quantity of practice for a suitable intervention arise on every occasion. For the same reason, a standing conclusion based on previous randomized clinical trials (RCT) could not be entirely generated. Two premises are considered vital for the implementation of SLT in aphasic patients, as seen in Figure 1 below [1,2]:
Based on the applied volume of rehabilitation, current terminology differentiates the following categories: “moderately intensive interventions” referring to a range between five to ten hours of speech-language therapy, and “highly-intensive interventions,” which apply more than ten hours of intensive practice per week [1].
For more insight into neurorehabilitation methods, check out:
- Home-based virtual-reality training improves functional recovery in chronic stroke and induces cortical reorganization
- Robot-assisted neurocognitive rehabilitation of the hand
- The feasibility of repetitive sensory stimulation in the rehabilitation of the upper limb after a stroke (the PULSE-I study)
- Accelerating the process of rehabilitation through virtual reality: The standing point of Reh@Task in post-stroke disability
Increasing supporting evidence
Regarding intensive speech-language therapy, insufficient data has been obtained based on the present literature. Two recent studies (of which one was a randomized controlled trial) assessed the role of intensive Speech-Language Therapy in different experimental conditions. The RCT focused on a specific approach for aphasic stroke survivors, namely Constraint-Induced Aphasia Therapy (CIAT). One interventional group was trained in a highly intensive manner, with 16 hours of practice per week, within two weeks. Compared to the more conventional moderately-intensive type of SLT, which consisted of six to eight hours of training per week for approximately one month (four to five weeks), the CIAT method expressed superior results in terms of speech improvement. However, the RCT above-mentioned could be considered moderate evidence, as it did not match the treatment protocol and the clinical background [3]. The second study mentioned above (a non-randomized study) addressed an identical issue, respectively, the moderately-intensive Speech-Language Therapy – 6 hours each week, for a total of 8 weeks – compared to highly-intensive Speech-Language Therapy – 16 hours each week, for a total of two months. The implied methodology can be considered questionable, as it did not randomly distribute the study population to treatment groups, therefore impacting the outcome on the suitable amount of overall practice (considering that both the quantity of weekly practice and the training interval were affected) [4].
The role of specific therapies – Introducing Intensive Language-Action Therapy (ILAT)
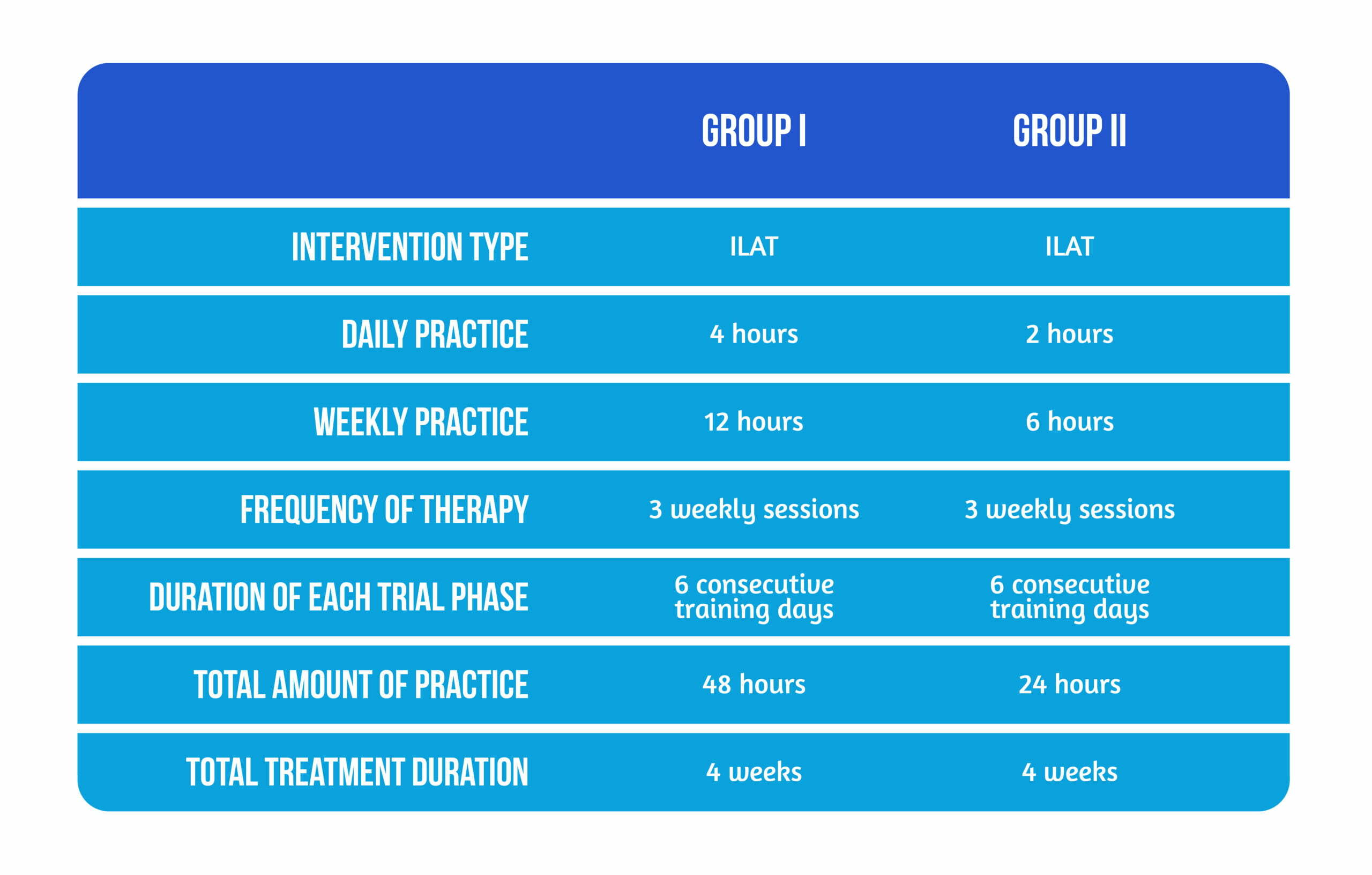
The RCT published by Stahl et al. in 2018 [1] used an extended version of the Constrained-Induced Aphasia Therapy, namely the ILA Therapy method, which was applied using different volumes of intensive rehabilitation practice. Two practices were subsequently compared: 12 hours of weekly aphasia training and training of 6 hours per week. As a result, the minimum acceptable dose of 5 to 10 hours (per week) was attained. Matched procedural and protocol aspects were used, addressing the previous methodological issues that could arise from the SLT studies mentioned above [4,5]. The entire study population had to go through three different periods: One waiting interval (the initial period) and two training periods that succeeded each other (with each intensive practice period encompassing two weeks). Further, the study population was equally divided into two interventional groups. Group I consisted of 15 patients who underwent 4 hours of daily intensive training, while the 15 patients in Group II performed 2 hours of training each day. ILAT was applied to both groups. The respective number of hours was grouped into three weekly sessions. All the patients completed the sessions without receiving any other form of speech therapy during the study [1].
The eligibility criteria for the patients are presented in Figure 2 below:

The diagnostic processes and application of the inclusion and exclusion criteria were assigned to a team consisting of a neuroscientist and a clinical linguist. The ischemic event was confirmed using MRI studies, with the lesion location comprising both cortical (left frontal, parietal, and temporal lobes) and subcortical regions [1].
The methodology behind ILAT required the engagement of patients in complex social group activities. A standard group consisted of three seated patients and a therapist. Illustrated cards (with different everyday actions or objects) were given to the patients. The subjects could not see the cards provided for their colleagues, as each card was distributed with a duplicate in possession of another player. The setting is illustrated in Figure 3. The main objective of the activity was for one of the players to gain possession of the matching card from their colleagues by asking for the specified object or by describing the action depicted. The complexity of the illustrations varied based on the patient’s skills in terms of language proficiency [1].

Three hundred thirty-six cards were available to the patients, with a card set including 12 illustrations. Various types of nouns (e.g., based on phonological similitudes or the number of word family members) and verbs (e.g., action-related verbs) were included. The assigned therapist’s roles were to encourage players’ progress and exemplify the use of specific actions of words in different contexts. Approval of gestures was present without replacing spoken language [1].
Different outcomes measures, similar results
The primary measure used by Stahl et al. was the Aachen Aphasia Test, which encompassed four subscales out of the six possible: Repetition, Naming, Comprehension, and the Token Test. In addition, two subscales were excluded: The Spontaneous Speech Scale, since it did not have enough construct validity, and the Writing Scale, as the respective study focuses mainly on spoken language. While no progress in terms of performance could have been observed during the study waiting period, a convincing improvement after each training interval was recorded, all independently regarding the level of difficulty of the session [1].
The second outcome measure applied was a novel psychometric scale, the Action Communication Test (ACT). The ACT was preferred as it is more impairment-focused than other instruments used to assess aphasia. It consists of two stages: during the first one, five physical objects are located in front of the patient. The patient’s task is to name all the natural objects presented to him. For the second stage, the subject requests the respective objects in the same order. If the patient’s verbal response matches the description of the requested object, then that object is handed to the patient (who collects them in a specially assigned bag). Fifty objects were used for the experimental conditions of the study. The ACT scale emphasized the results recorded after the appliance of the first outcome measure, the only difference being the interruption of the highly-intensive SLT group progress during the second training session [1].
No differences were recorded based on the AAT and ACT scores at baseline or regarding differences in the following variables: age, level of education, the number of months that have passed since the ischemic incident, short-term memory (non-verbal), and the size of the injury on the MRI [1].
Further directions
A classical neuroscientific theory, known as the cell assembly theory (or Hebb’s rule – ‘’Cells that fire together wire together’’), postulates the amount of stimulation a postsynaptic cell receives from a presynaptic one conditions the efficiency of that synapse. Superimposing Hebb’s model on the study performed by Stahl et al., the theory suggests that while daily training of the aphasic patients can impact the reorganizational aspects of language, a ceiling effect can not be ruled out as an obstacle, therefore limiting the effect of the therapy, independent of the amount of practice that a patient receives daily.
Based on the RCT results published by Stahl et al., the maximum amount of training that should be administered to aphasic patients as a rehabilitation method should not exceed 2 hours each day. A 2-hour per day dose of intensive therapy is subsequently considered sufficient, increasing the patients’ adherence to the rehabilitation process. Nevertheless, an extended time interval could be beneficial for patients that struggle with the above-mentioned speech impairment (with a minimum increase of two weeks being considered significant). In conclusion, the rehabilitation process of post-stroke speech impairments could be facilitated by similar results of future RCTs, reducing time-consuming processes to recover function in different conditions (e.g., dysarthria).
Post-stroke aphasia can be considered a volatile condition that severely impacts patients’ quality of life (QOL), with little knowledge available regarding the amount of time necessary for improvement or regression of symptomatology. Therefore, as it offers valuable information in the field of neurorehabilitation, it can be considered that the work of Stahl et al. generated necessary evidence for the optimal cut-off points of the time interval for aphasia interventions (addressing both daily practice and the total amount of time) [1].
References
- Stahl B, Mohr B, Büscher V,Dreyer FR, et al. J Neurol Neurosurg Psychiatry 2018;89:586–592. DOI: 10.1136/jnnp-2017-315962
- Cherney LR, Patterson JP, Raymer A, Frymark T, et al. Evidence-based systematic review: effects of intensity of treatment and Constraint-Induced Language Therapy for individuals with stroke-induced aphasia. J Speech Lang Hear Res 2008;51:1282–99. DOI: 10.1044/1092-4388(2008/07-0206)
- Pulvermüller F, Neininger B, Elbert T, Mohr B, et al. Constraint-induced therapy of chronic aphasia after stroke. Stroke 2001;32:1621–6. DOI: 10.1161/01.str.32.7.1621
- Dignam J, Copland D, McKinnon E, Burfein P, et al. Intensive versus distributed aphasia therapy: a non-randomized, parallel-group, dosage-controlled study. Stroke 2015;46:2206–11. DOI: 10.1161/STROKEAHA.115.009522
- Difrancesco S, Pulvermüller F & Mohr B. Intensive Language-Action Therapy (ILAT): the methods. Aphasiology 2012. 26. 1-35. DOI 10.1080/02687038.2012.705815.










One thought on “Shedding light on Speech-Language Therapy: How stroke survivors can benefit from intensive rehabilitation training for chronic aphasia”